|
Acute Respiratory Distress Syndrome
Adult Respiratory Distress Syndrome
Rapidly
developing respiratory insufficiency resulting from leakage of protein-rich
edema fluid into the alveoli 2° damage to the capillary endothelium
•
Synonyms: Shock
lung, non-cardiogenic pulmonary edema, post-traumatic pulmonary insufficiency,
pump lung, stiff lung syndrome, respirator lung, hemorrhagic lung
•
Constellation of Signs and Symptoms
•
Tachypnea, dyspnea, cough
• Diffuse air-space disease on chest x-ray
• Severe arterial desaturation resistant to high concentrations of
inhaled 02
• Pulmonary function tests showing increased pulmonary vascular
pressures and resistances and decreased compliance
•
Predisposing conditions:
•
Shock
• Hypovolemic, hemorrhagic
• Septic-especially gram negative
•
Burns
•
Massive aspiration of gastric contents (Mendelssohn’s Syndrome)
•
Acute pancreatitis
•
Heroin/methadone/crack cocaine overdose
•
Disseminated intravascular coagulation
•
Smoke, chlorine gas, nitrogen dioxide inhalation
•
Massive viral pneumonia
•
Fat embolism
•
Near-drowning
•
Pathology
• Diffuse alveolar damage
• Damage to type I pneumocytes produces flooding of alveoli with
edema fluid
• Hyaline membranes form and line distal airways and alveoli
• Type II pneumocytes proliferate to reline denuded alveolar surfaces
• Fibroblastic tissue is generated in and around airspaces
•
Imaging Findings
• No cardiomegaly
• No pleural effusions
• No Kerley B lines
• Delay in onset of any x-ray findings for at least 12 hours
post-insult
• Between 12 and 24 hours
• Patchy alveolar infiltrates in both lungs
• Between 24 and 48 hours
• Coalesce to produce massive air-space consolidation of both lungs
• From 5 to 7 days
• Clearing is frequently 2° effects of CPP ventilation rather than
true healing
• Pneumonia may superimpose
• Difficult to recognize but look for new focal infiltrates and
pleural effusion
• More than one week
• Coarse reticular interstitial disease which may lead to fibrosis
•
Complications of CPP ventilation
• Pneumothorax
• Pneumomediastinum
• Pulmonary interstitial emphysema
•
Differential Diagnosis
• Severe bacterial pneumonia--impossible to differentiate except
clinically
• Other forms of pulmonary edema (see below)
|
Cardiogenic
|
Renal
|
ARDS
|
Distribution
of Pulmonary edema
|
90%
even
|
70%
central
|
45%
Peripheral
35% Even
|
Kerley
B lines/ peribronchial cuffing
|
30%
|
30%
|
None
|
Pleural
effusions
|
40%
|
30%
|
10%
|
Air
bronchograms
|
20%
|
20%
|
70%
|
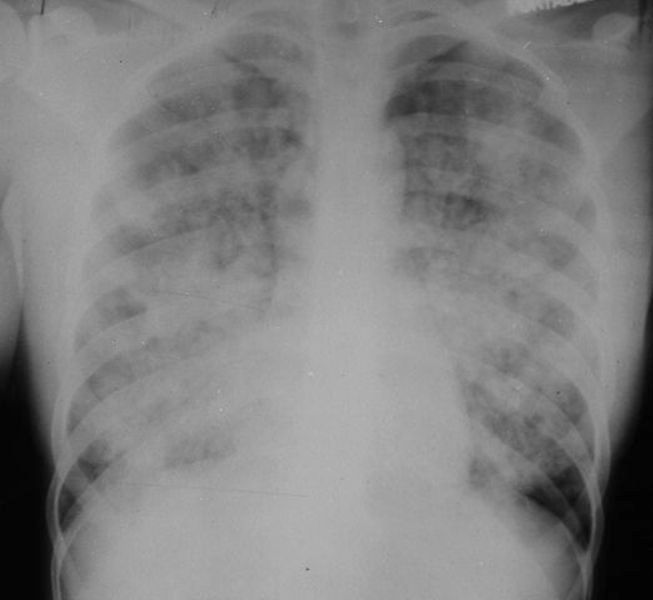
Adult Respiratory Distress Syndrome. There are diffuse, bilateral airspace disease without pleural effusions or cardiomegaly. The person was involved in a near-drowning.
|