|
Renal Osteodystrophy
Rugger-Jersey Spine
· Constellation of musculoskeletal abnormalities
occurring with chronic renal failure featuring some combination of
o Osteomalacia (adults)
o Rickets (children)
o 2° hyperparathyroidism
o Soft-tissue calcifications
o Osteosclerosis
o Soft-tissue + vascular calcifications
· Low calcium levels lead to osteomalacia
o Additional factors responsible for osteomalacia are
§ Inhibitors to calcification produced in the uremic
state
§ Aluminum toxicity
§ Dysfunction of hepatic enzyme system A
§ Renal insufficiency with diminished filtration results
in phosphate retention
· Maintenance of Ca x P product lowers serum calcium
directly, which in turn increases parathyroid hormone production
(2°hyperparathyroidism)
· Osteopenia
o Combined effect of
§ Osteomalacia (reduced bone mineralization due to
acquired insensitivity to vitamin D / antivitamin D factor)
§ Osteitis fibrosa cystica (bone resorption)
§ Osteoporosis (decrease in bone quantity)
o Complications
§ Fracture predisposition (lessened structural strength)
with minor trauma
· Spontaneously
§ Fracture prevalence increases with duration of
hemodialysis + remains unchanged after renal transplantation
· Sites of fractures
o Vertebral body (3-25%)
o Pubic ramus, rib (5-25%)
o Milkman fracture / Looser zones (in 1%)
o Metaphyseal fractures
o Prognosis
§ Osteopenia may remain unchanged / worsen after renal
transplantation + during hemodialysis
· Secondary hyperparathyroidism
o Cause
§ Inability of kidneys to adequately excrete phosphate
leads to hyperplasia of parathyroid chief cells (2°
hyperparathyroidism)
§ Excess parathyroid hormone affects the development of
osteoclasts, osteoblasts, osteocytes
o Hyperphosphatemia
o Hypocalcemia
o Increased PTH levels
o Subperiosteal, cortical, subchondral, trabecular,
endosteal, subligamentous bone resorption
o Osteoclastoma = brown tumor = osteitis fibrosa cystica
(due to parathyroid hormone -stimulated osteoclastic activity
§ More common in 1° hyperparathyroidism
o Periosteal new-bone formation (8-25%)
o Chondrocalcinosis
§ More common in 1° hyperparathyroidism)
· Osteosclerosis (9-34%)
o One of the most common radiologic manifestations
§ Most common with chronic glomerulonephritis
o May be the sole manifestation of renal osteodystrophy
o Diffuse chalky density
o Thoracolumbar spine in 60% with dense end-plates
produce appearance of rugger-jersey (rugger jersey spine)
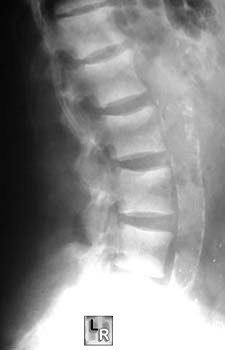
Rugger-jersey spine in
Renal osteodystrophy
o Also in pelvis, ribs, long bones, facial bones, base
of skull (children)
o Prognosis
§ May increase/regress after renal transplantation
· Soft-tissue calcifications
o Metastatic secondary to hyperphosphatemia (solubility
product for calcium + phosphate exceeds 60-75 mg/dL in extracellular
fluid)
§ Hypercalcemia
§ Alkalosis with precipitation of calcium salts
o Dystrophic secondary to local tissue injury
§ Location
· Arterial (27-83%)
o In medial + intimal elastic tissue
§ Dorsalis pedis a., forearm, hand, wrist, leg
o Pipestem appearance without prominent luminal
involvement
· Periarticular (0-52%)
o Multifocal
o Frequently symmetric
o May extend into adjacent joint
o Chalky fluid / pastelike material
o Inflammatory response in surrounding tenosynovial
tissue
o Discrete cloudlike dense areas
§ Fluid-fluid level in tumoral calcinosis
o Prognosis
§ Often regresses with treatment
· Treatment
o Decrease of phosphorus absorption in bowel
o Vitamin D3 administration (if vitamin D resistance
predominates)
o Parathyroidectomy for 3° hyperparathyroidism (=
autonomous hyperparathyroidism)
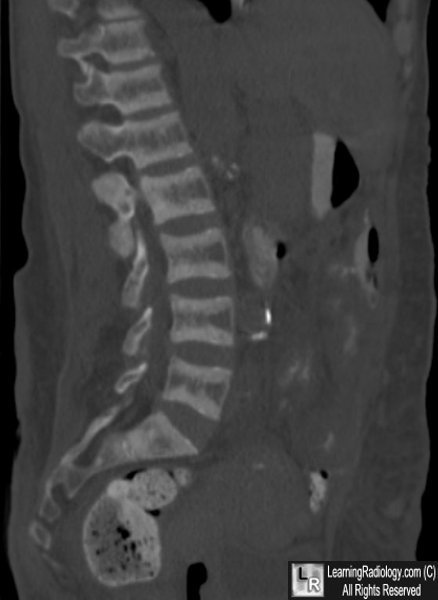
Rugger Jersey Spine in Renal Osteodystrophy. Sagittal CT reconstruction of spine shows alternating bands of increased density at the endplates of vertebral bodies and less dense central portions.
|